Section Guide
6 Sections
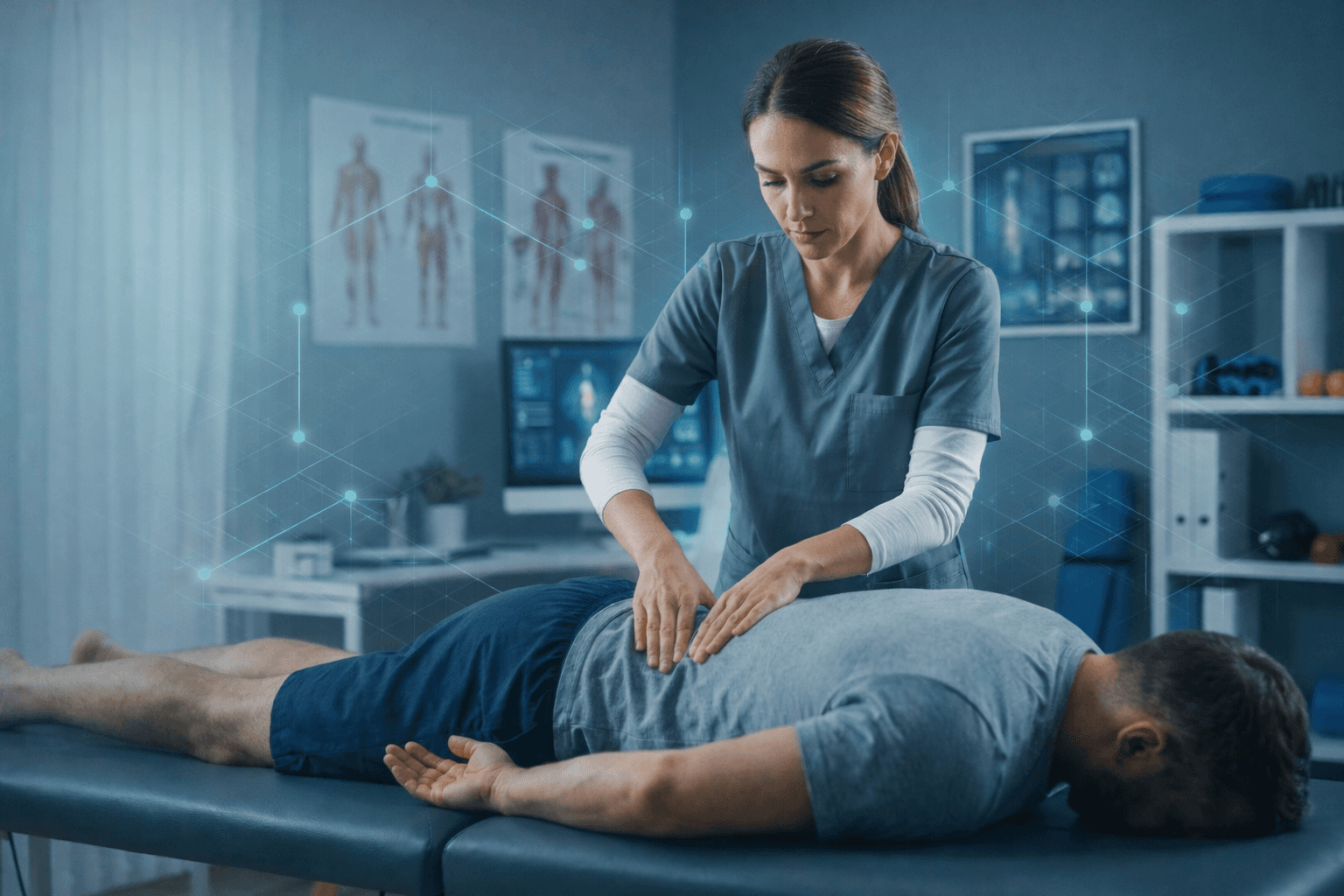
Function-focused rehabilitation for persistent pain, movement sensitivity, flare-up anxiety, and reduced confidence with daily activity.
Section Guide
6 Sections
This section explains how symptoms typically behave, what often keeps them going, and which physical capacities usually need to improve for recovery to hold up in daily life.
Chronic pain syndrome usually involves pain that has stayed active for longer than expected and is now affecting sleep, energy, confidence, work, and normal activity levels. In many cases the nervous system has become more protective and symptoms can feel out of proportion to day-to-day loading.
Rehabilitation is not about dismissing the pain. It is about understanding how pain sensitivity, stress, pacing, conditioning, and activity avoidance are interacting so function can begin to improve again.
Clinical Snapshot
Function-focused rehabilitation for persistent pain, movement sensitivity, flare-up anxiety, and reduced confidence with daily activity.
Typical Symptom Pattern
What We Clarify During Assessment
Related Guides
If your symptoms feel more specific or overlap with another pattern, these guides can help you understand the closest condition pathways.
Fibromyalgia
Graded rehabilitation support for widespread pain, fatigue, sensitivity, and difficulty maintaining everyday activity with fibromyalgia.
Back Pain
Assessment-led physiotherapy for mechanical low back pain, recurrent flare-ups, stiffness, and load-related lumbar symptoms.
Neck Pain
Targeted physiotherapy for neck pain, stiffness, desk-related strain, and movement-linked cervical flare-ups.
We identify where the pain cycle is being reinforced by fear, avoidance, overdoing on good days, underdoing on bad days, or poor recovery. That gives us a more realistic starting point for progression.
Treatment then aims to rebuild tolerance and confidence steadily, using meaningful functional goals instead of chasing complete symptom removal before activity resumes.
Your Plan May Include
No. The pain is real, but long-standing pain often involves a more sensitive protective system, which changes how recovery needs to be managed.
Yes, when it is introduced gradually and matched to your current tolerance. The goal is to rebuild confidence and function without repeated big flare-ups.
Progress can include better sleep, longer walking tolerance, more confidence, fewer big flare-ups, and improved ability to work or exercise even before pain is fully settled.