If you have ever experienced pain, you have probably assumed — quite reasonably — that something in your body is broken, torn, or damaged. It is one of the most deeply held beliefs about pain: that it is a direct readout of physical harm. But modern pain science tells a very different story. Pain is not simply an alarm bell ringing at the site of an injury. It is far more complex, far more personal, and — importantly — far more manageable once you understand how it actually works.
The Common Misconception: Pain Equals Damage
For most of human history, pain was understood through what is known as the "Cartesian model" — named after the philosopher René Descartes, who imagined pain as a simple pipeline. Damage occurs in the body, a signal travels up to the brain, and pain is felt. The more damage, the more pain. Simple, logical, and unfortunately, wrong.
This model has been thoroughly overturned by decades of neuroscience research. We now know that pain and tissue damage are two separate things that can — and often do — occur independently of each other. Understanding this distinction is not just an academic exercise. It has real, practical implications for how you recover, how you move, and how much fear you carry around your symptoms.
What Is Pain, Really?
The International Association for the Study of Pain defines pain as "an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage." Notice the key phrase: potential tissue damage. Pain does not require actual harm to occur.
A more useful way to think about pain is this: pain is a protective output produced by the brain. Its purpose is to motivate you to do something — to rest, to seek help, to avoid a dangerous situation. Pain is the brain's best guess that your body is in danger and that action is needed. It is a decision, not a measurement.
This reframing is powerful. It means that pain is always real — it is never "just in your head" in a dismissive sense — but it is also always produced by the nervous system, not by the tissue itself. Your experience of pain is genuine and valid, regardless of what a scan does or does not show.
The Role of the Brain: From Danger Signals to Pain
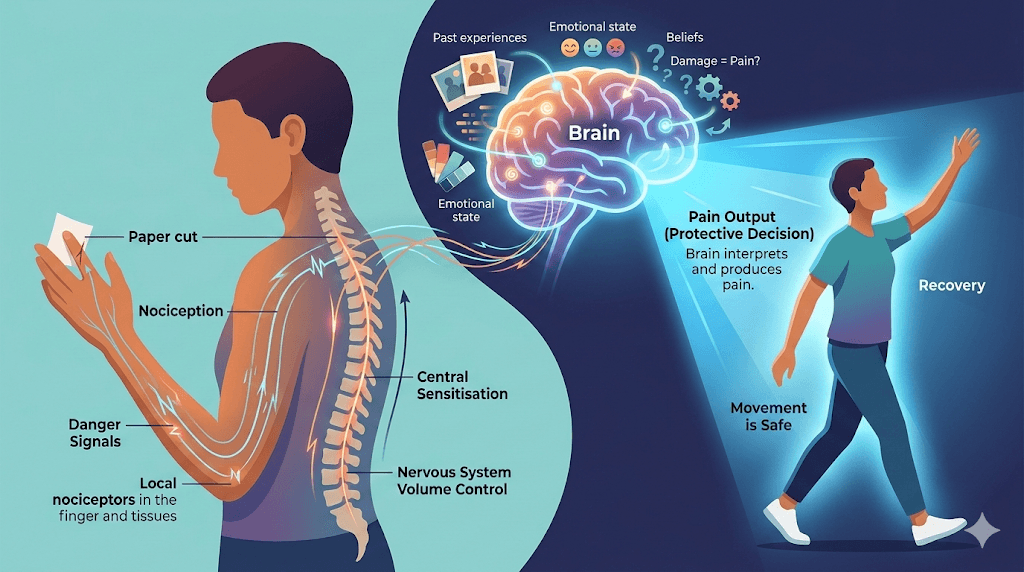
Your body is filled with specialised nerve endings called nociceptors. These are danger detectors — they respond to potentially harmful stimuli such as extreme heat, pressure, or chemical changes associated with tissue stress. When activated, they send signals up through the spinal cord to the brain. This process is called nociception.
Here is the critical point: nociception is not pain. Nociception is the raw data — the danger signal. Pain is the brain's interpretation of that data, weighed against everything else it knows about the situation. The brain asks, in effect: "Is this body part actually in danger? Do I need to protect it?"
To answer that question, the brain draws on a vast range of information: the context you are in, your past experiences with pain, your beliefs about what is happening, your emotional state, your stress levels, and even your expectations. All of this shapes whether pain is produced, and how intense it feels. Two people with identical injuries can have vastly different pain experiences — and both are completely valid.
Pain and Tissue Damage: Why They Don't Always Match
Once you understand that pain is a brain output rather than a tissue signal, the mismatch between pain and damage starts to make sense. Consider these everyday examples:
A paper cut on your fingertip can be agonising, yet the actual tissue damage is minuscule. The fingertip is densely packed with nerve endings and is critical for fine motor tasks — so the brain treats even minor threats there as high priority.
Soldiers and athletes in the heat of competition have sustained serious injuries — broken bones, deep lacerations — and felt little or no pain until the event was over. The brain, focused on survival or performance, deprioritised the pain signal.
Phantom limb pain is perhaps the most striking example. People who have had a limb amputated can experience intense, ongoing pain in the missing limb. There is no tissue to be damaged — yet the pain is absolutely real. The brain continues to produce pain in the absence of any physical structure.
These examples are not anomalies. They are windows into how pain actually works. Pain is always a product of the nervous system — and the nervous system is influenced by far more than just what is happening in your tissues.
Why Scans and Tests Don't Always Explain Your Pain
One of the most distressing experiences for people in pain is being told that their scan "looks fine" — or conversely, being shown a scan full of findings and assuming the worst. Neither situation is as straightforward as it seems.
Research consistently shows that structural findings on imaging — such as disc bulges, disc degeneration, facet joint changes, rotator cuff tears, and knee osteoarthritis — are extremely common in people who have no pain at all. A landmark study published in the American Journal of Neuroradiology found that by the age of 50, over 80% of people with no back pain had disc degeneration visible on MRI. By age 70, that figure approached 90%.
This does not mean scans are useless — they are essential for ruling out serious pathology. But it does mean that a finding on a scan is not automatically the cause of your pain. Many people carry these structural changes throughout their lives without ever knowing, because their brain never decides those changes are threatening enough to produce pain.
Conversely, some people experience significant pain with very little structural change visible on imaging. This is not a sign that their pain is imagined or exaggerated — it is a sign that the nervous system is playing a larger role than the tissue.
Sensitisation: When the Nervous System Turns Up the Volume
One of the most important concepts in understanding persistent pain is sensitisation. When pain continues over weeks and months, the nervous system can undergo changes that make it more reactive — essentially turning up the volume on danger signals.
There are two main types. Peripheral sensitisation occurs at the site of injury or inflammation, where local nerve endings become more sensitive and fire more easily. This is why a sunburned shoulder hurts when you put on a shirt — the threshold for triggering a pain response has been lowered locally.
Central sensitisation occurs within the spinal cord and brain itself. The central nervous system becomes amplified, processing normal or even non-threatening signals as if they were dangerous. This can explain why pain spreads beyond the original injury site, why light touch becomes painful, and why pain persists long after tissues have healed.
Sensitisation is not a sign of weakness or psychological fragility. It is a physiological process — a nervous system that has learned, through repeated experience, to be on high alert. The good news is that just as the nervous system can learn to be more sensitive, it can also learn to calm down.
What This Means for Your Recovery
Understanding pain science is not just intellectually interesting — it has direct, practical benefits for recovery. Research shows that people who understand how pain works report lower pain levels, less disability, and greater confidence in moving their bodies. This is sometimes called "pain neuroscience education" or PNE, and it is now a well-established component of effective pain management.
One of the most important shifts that comes from this understanding is a reduction in fear. When you believe that pain always means damage, every twinge during movement feels like a warning to stop. This fear of movement — known clinically as kinesiophobia — can lead to avoidance, deconditioning, and a worsening of pain over time. It becomes a self-reinforcing cycle.
When you understand that pain is a protective signal rather than a damage report, movement becomes less threatening. Gentle, graded activity — gradually increasing what you do over time — is one of the most effective tools for reducing sensitisation and rebuilding confidence. Movement is not the enemy of recovery. In most cases, it is one of the most powerful medicines available.
This does not mean pushing through severe pain or ignoring your body. It means working with a qualified clinician to find a level of activity that is manageable and gradually expanding from there. The goal is to help your nervous system learn that movement is safe — and over time, that message tends to reduce pain.
Understanding Pain Is the First Step to Managing It
Pain is one of the most complex and personal experiences a human being can have. It is shaped by biology, psychology, history, context, and meaning. It is always real. It is always worth taking seriously. And it is almost always more changeable than it feels in the moment.
The old model — pain equals damage — left many people feeling helpless, afraid to move, and confused when their scans didn't match their experience. The new understanding of pain offers something far more empowering: a framework in which you are not a passive victim of your tissues, but an active participant in your own recovery.
If you are living with pain, know this: your pain is real, your experience is valid, and there are effective, evidence-based approaches to help you move forward. Understanding how pain works is not a cure — but it is a genuinely powerful first step. And first steps, as anyone who has recovered from pain will tell you, matter enormously.