Diabetic neuropathy is often misunderstood as “just numbness in the feet.” In reality, it can significantly alter walking mechanics, balance, and coordination. Over time, this raises the risk of falls, skin breakdown, and reduced independence. Early intervention matters.
At Physynex, neuropathy management includes movement testing, sensory screening, gait analysis, and functional loading guidance. If you have symptoms and want a personalized plan, use our Contact Page (https://www.physynex.in/contact) to schedule an assessment.
Common signs patients ignore
burning or tingling in feet, especially at night
reduced ability to sense ground contact
frequent imbalance or tripping
slower walking and shorter step length
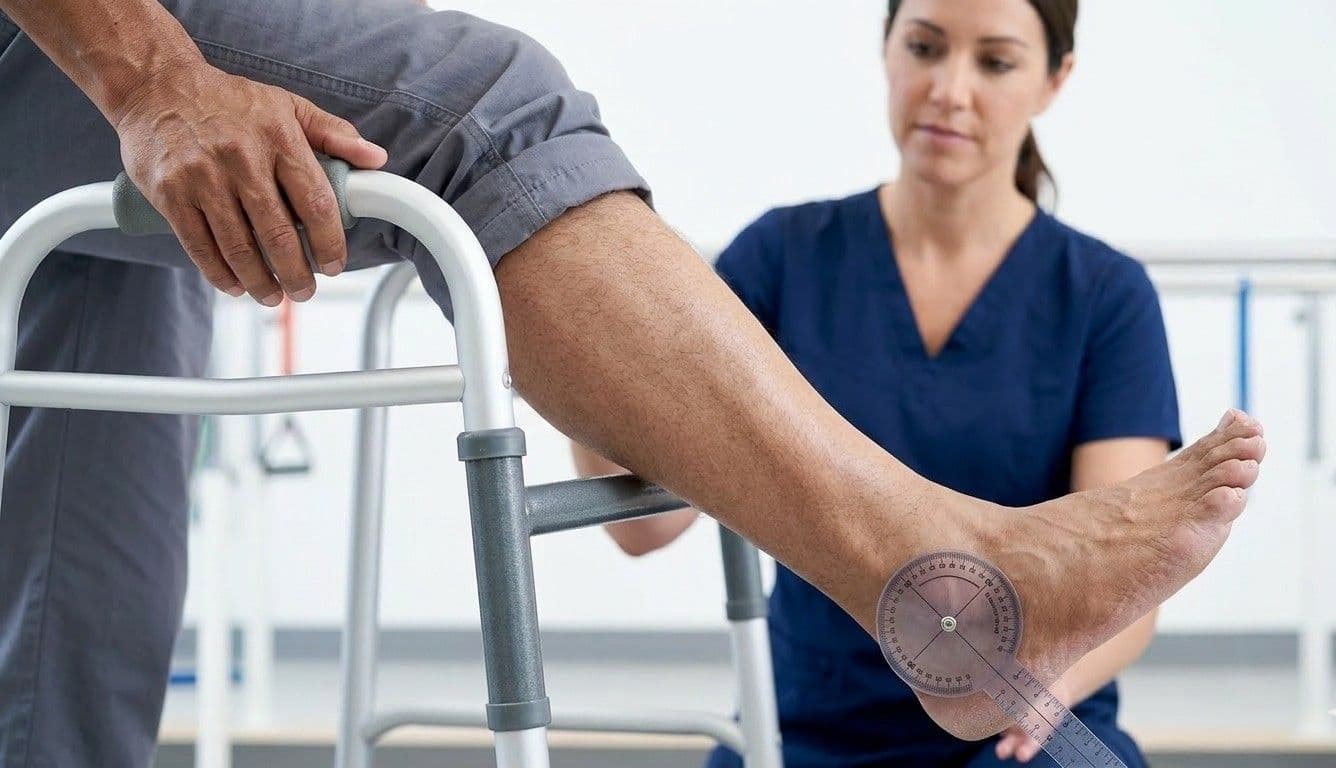
ankle weakness and instability
If these symptoms are present, waiting can make recovery harder. Our Diabetic Neuropathy Condition Page (https://www.physynex.in/conditions/leg-ankle-and-foot-pain) and Diabetic Foot article pathway (https://www.physynex.in/blog) are useful starting points for understanding next steps.
How physiotherapy helps
A strong plan focuses on both protection and progression:
balance and proprioception training
lower limb strengthening
gait retraining for safer movement
ankle mobility and calf capacity work
foot-loading education to reduce tissue risk
This is often integrated with Manual Therapy (https://www.physynex.in/services/manual-therapy) and functional progression strategies from Sports Rehabilitation principles (https://www.physynex.in/services/sports-rehabilitation), adapted for non-athlete populations.
Why movement care is essential in neuropathy
When sensation drops, people naturally move less. But reduced movement leads to deconditioning, slower reaction time, and poorer circulation. A guided mobility program helps break this cycle and supports safer, more confident daily function.
Red flags needing urgent review
new wounds or blisters that do not heal
increasing redness or swelling
sudden weakness or sharp changes in walking
repeated falls or near-falls
Neuropathy care should be proactive, not reactive. Early physiotherapy improves long-term mobility outcomes and helps reduce avoidable complications.

